A nationally recognized health care plan provider is an industry leader in providing member-centric health care coverage. The company’s managed care business model is one of the nation’s largest Medicaid managed care plans.

Health Care Plan Provider - Care Management
Challenge
Every member of this health care plan is assigned a Care Manager with a supporting team. The team can be comprised of nurses, social workers, and navigators. Their goal is to understand member needs, and help them meet their goals for a healthy life. To support a growing number of members across multiple states, this health care plan provider determined to improve the efficiency and effectiveness of tools used by the care teams.
Solution
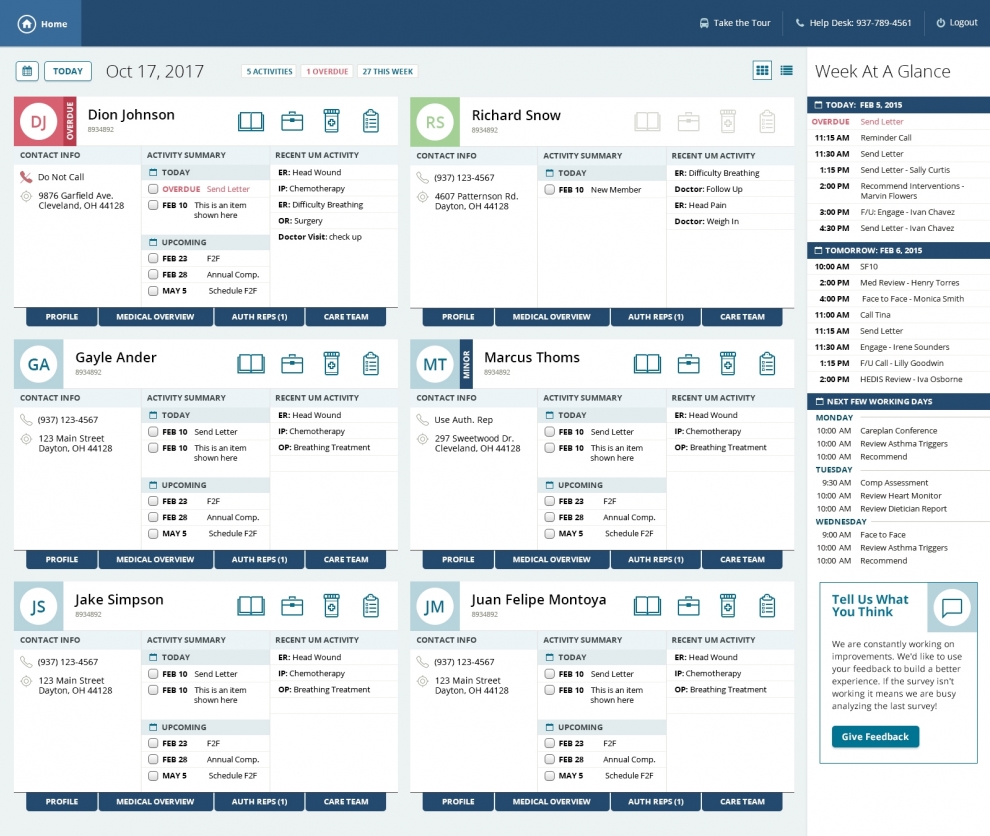
This health care plan provider developed a care management tool that enabled care managers to quickly understand their tasks for the day and efficiently form a comprehensive view of a members current situation.
An interdisciplinary POMIET team was engaged to research, design, and prototype a user interface that supports the care management process. Our UX researchers and designers worked closely with care managers from around the country to understand their workflow, and iteratively designed highly efficient solutions.
A significant constraint to address was to support members who moved frequently or changed phone numbers. POMIET data scientists worked jointly with the client’s data team to understand how the data could be used to provide a comprehensive solution for care managers to locate these transient members.
The result of this interdisciplinary approach is a system with an impressive System Usability Score (SUS) of 93 (out of 100).
Publications
Reducing Stress in Healthcare Using an Integration Design Model http://journals.sagepub.com/doi...
Computer as Partner: A Synergistic Approach to Interaction Design http://uxmag.com/articles/computer-as-partn...
This is a great team to work with. Each person is top-notch and easy to collaborate with. You guys just get it, and do exceptional work.
Gillian Fraser eNeura Therapeutics
Looking for a guide on your journey?
Ready to explore how human-machine teaming can help to solve your complex problems? Let's talk. We're excited to hear your ideas and see where we can assist.
Let's Talk